The integration of intelligent automation and AI in point-of-care testing to enhance healthcare delivery. It focuses on the digitization of the NHS Health Check program through remote consultations, monitoring, and diagnostics. By utilizing AI-driven tools, such as automated ECG analysis and blood pressure monitoring, the program improves accessibility, efficiency, and preventive care.

Over the past two decades, advances in technology have revolutionized healthcare delivery worldwide. From telemedicine to artificial intelligence (AI), these innovations have transformed the patient experience, improved access to care, and driven efficiencies across healthcare systems. Technology-enabled care (TEC) now plays a pivotal role in addressing global health challenges, from managing chronic diseases to tackling pandemics however, given the global challenges in delivering healthcare to a growing and ageing population with multiple co-morbidities technology can, should and will need to ensure a sustainable health system.
Whilst technology enabled care covers a broad spectrum of technology and applications in practice, this article will explore the 3 x R’s; remote consultations, remote monitoring and remote diagnostics and how combined we can digitize one of the oldest and most successful cardiovascular prevention programmes in the world utilising cutting edge technology.
One of the most significant advancements in TEC is the widespread adoption of telemedicine. Although, the first application of telemedicine can be attributed to the University of Nebraska in 1959, telemedicine didn’t truly find its place in mainstream healthcare until the Covid Pandemic. Within 3 months of the first lockdown in the UK, 85% of the population had access to remote consultations from health providers and within 6 months, this had increased to 99%.
The earliest example of remote monitoring was in 1961 where the first man in space, Alan Shepard was able to transmit biological data to NASA however, similarly to the growth of remote consultations, health providers didn’t see the full benefit until the Covid pandemic. We are now seeing a wide variety of applications for remote monitoring and the advancement in continuous monitoring wearables now allows patients vital signs to be monitored using medically certified devices. This is further being enhanced by the application of artificial intelligence which combined with intelligent automation can be utilised for automating ECG analysis or predicting early signs of Sepsis.
The first instance of remote diagnostics can be attributed to Del Mar Engineering Laboratories in 1967 where they utilised the traditional ECG Holter to transmit EKG signals over the telephone. Point of care testing began in the early 1980’s which started with blood samples analysed from patients undergoing hepatic transplantation at the University of California. Remote diagnostics and point of care testing are becoming a growing industry given its ability to enable faster, more accessible, and efficient diagnostics without the need for traditional laboratory settings or lengthy hospital visits.
Cardiovascular disease (CVD) is the leading cause of death globally and beyond its devastating toll on individuals and families is responsible for approximately 17.9 million deaths annually - 31% of all global deaths, according to the World Health Organization. The economic ramifications are staggering with the global cost for treating CVD estimated to be above $1 trillion with predictions this figure will rise as population’s age and risk factors such as obesity, hypertension and diabetes become more prevalent. In the UK, Public Health England have calculated that outside direct healthcare costs, it is estimated that CVD costs the UK economy £15.8 billion per year.
Cardiovascular disease of course is largely preventable with the British Heart Foundation stating that 80% of all cardiovascular disease is preventable.
The NHS Health Check programme commenced in 2009 and is a 20 – 30 minute assessment traditionally undertaken in clinic for 40 – 74 year olds aiming to identify early signs of health issues such as CVD, Diabetes and chronic kidney disease. During the health check, patients will answer health and lifestyle questions, have their blood pressure and BMI measured whilst undertaking blood tests for cholesterol levels.
NHS data shows that, while millions are eligible for the Health Check annually, not all take advantage of the offer. Only 25% of eligible individuals attended an NHS Health Check in the last 5 years with variation between 10 – 50% across regions in the UK. The reasons for this vary with public awareness, access challenges due to lack of flexibility for appointments, scheduling conflicts, geographical barriers, health literacy and perceived healthiness. It is estimated that in the UK today:-
- 8 million people are living with undiagnosed or uncontrolled blood pressure
- 1.2 million people are likely to have undiagnosed type 2 diabetes
- 50% of all adults are living with cholesterol levels above national guidelines for total cholesterol
- 38% of adults have a BMI defined as overweight
- 37% of adults do not meet physical activity recommendations
To rectify the health check deficit, it is estimated that 1,818 healthcare professionals would need to work solely on delivering health checks as well as over 7 million pathology requests. All of this whilst a Kings Fund reports 121,000 full time equivalent health professional vacancies across the NHS.
When breaking down the components of the health check process workflow, we have:-
- An appointment booking request which is initiated from the Practice and we know the uptake is low
- A face to face appointment with a healthcare professional which will consist of:-
• Health and Lifestyle questionnaire
• Weight measurement
• Height measurement
• Maximum of 2 x blood tests
- The output of the appointment (once all results are received) will be:-
• A health report
• Sign-posting to services and information relating to health and lifestyle
• Potential referral onto other clinicians for example, chronic disease nurse
• Potential requirement for further monitoring for example, blood pressure monitoring either for 7 days or ambulatory 24 hour
Utilising the 3 x R’s referenced earlier in this article a Cumbrian health provider utilised a combination of different health-tech solutions to digitize the NHS Health Check programme. The project was launched in conjunction with local government, local health providers and commissioned by the Department of Health and Social Care (DHSC) with a target of 9,000 employees to be screened.
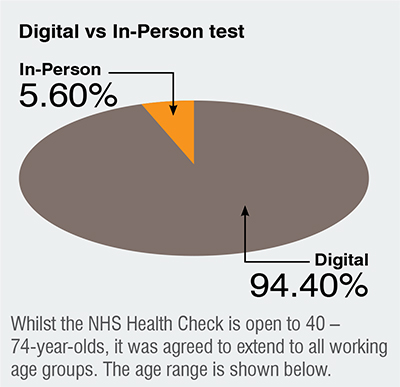
Employees would have the option of either a digital self-test which they would order themselves to their home address or attend a health check which would be delivered by a healthcare professional but utilising the same digital test.
The digital self-test contained the following components: -
- A lateral flow test cartridge
- A lancet
- A capillary tube
- A card with a QR code to download an app
Those choosing the face-to-face option would have the same test but, in their workplace, instead of their GP practice.
For those undertaking the digital self-test would: -
- Take delivery of the digital self-test either at home or in the workplace dependant on their choice of address
- Download the app using the QR code and register their details into the App.
- Complete the health and lifestyle questionnaire
- Use the lancet and capillary tube to take their own blood sample and insert into the test cartridge
- Wait 7 minutes for the blood sample to be analysed
- Be presented with their results which would also be emailed to them and their General Practice (GP)
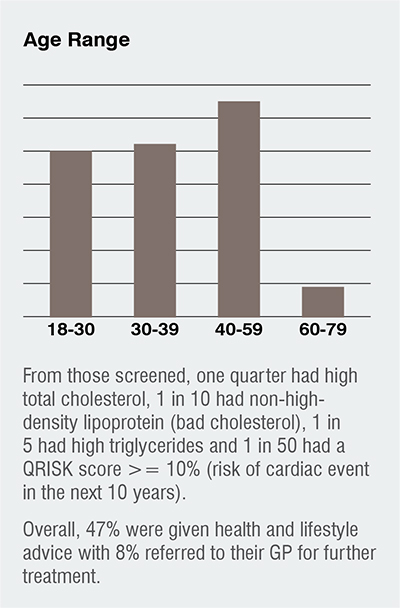
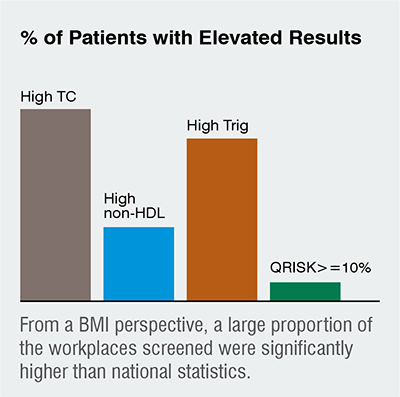
The app would direct all of the above steps with detailed instructions given at each stage and following the analysis of the results, the app (using App notifications) directs the patient to health and lifestyle advice based on their results should their results be out-with expected parameters for their demographics or specific responses to some questions for example, BMI out of range, high cholesterol, smoking status etc.
Any patients with an out-of-range blood pressure are offered the digital BP@Home service which would monitor them for 7 x successive days using an AI powered mobile application providing advice on out-of-range measurements whilst a 24 hour control room would monitor on a dashboard. At the end of the 7 days, a report would be sent to their GP practice for review.
Employees were offered video consultations with a healthcare professional on a secure web-based video consultation platform.
Employers were offered a health profile for their workplace alongside a suggested health action plan for dealing with the results for example, changes to in-house cafeteria options, targeted health campaigns, healthy living workshops etc.
The Health Check programme was a resounding success, particularly the Digital self-tests which were by far the most popular option amongst employees with only 1 in 20 staff preferring the face-to-face tests.