Ultrasound technology has revolutionized patient care, transitioning from stationary, bulky machines to today's portable handheld devices. These devices provide flexibility in medical settings, enabling quicker diagnoses and enhancing patient care. This evolution highlights a trend towards more accessible and efficient healthcare diagnostics.
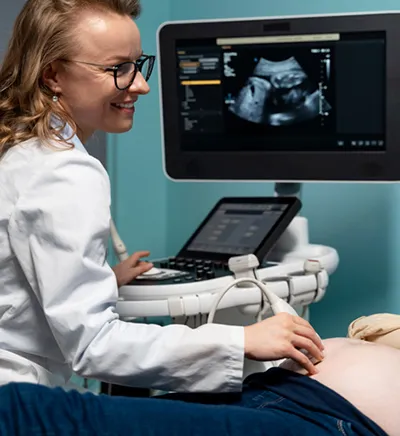
Ultrasound technology has undergone significant transformations since its inception. Originally, ultrasound machines were large, cumbersome, and expensive, typically housed in dedicated imaging rooms within hospitals (figure 1). These early devices were stationary and required trained technicians to operate, limiting their use primarily to specialized departments and settings. Advances in microelectronics, battery technology, and medical imaging software have dramatically transformed these devices over the past few decades. The development of portable ultrasound machines marked a significant step forward, allowing for greater flexibility in where and how ultrasounds could be performed. However, the most ground-breaking evolution has been the introduction of handheld ultrasound devices. These pocket-sized tools, equipped with high-resolution imaging capabilities, have revolutionized the field by providing real-time, on-the-go diagnostic capabilities.
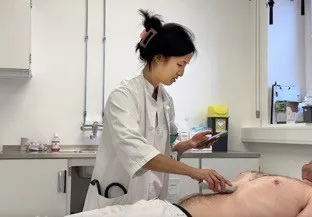
Handheld ultrasound devices offer several advantages over their larger predecessors (figure 2). The most obvious benefit is their size. Handheld devices can easily be carried in a doctor's pocket, making it possible to perform ultrasounds at the bedside, in emergency situations, or even in remote locations. Modern handheld devices are designed with user-friendly interfaces, often integrating touchscreen controls and intuitive software. This ease of use means that a broader range of healthcare professionals can operate the devices with minimal training. Handheld ultrasound devices are significantly less expensive than traditional machines. This lower cost can make ultrasound technology accessible to a wider range of healthcare settings, including small clinics and practices that might not have been able to afford traditional ultrasound machines.

Many studies show that portable handheld ultrasound devices are beneficial in different settings. This is where physicians use point-of-care ultrasound (POCUS). POCUS is an ultrasound examination performed by medical professionals at the bedside wherever a patient is being treated, whether that’s in a modern hospital, an ambulance, or a general practitioner’s office. The difference between a POCUS examiner and a radiologist is that medical professionals are answering yes or no questions: Is there the presence of pleural or pericardial effusion? Does the patient have heart failure? What about hydronephrosis? Does the patient have gallstones or any signs of acute cholecystitis? Handheld ultrasound devices are not just for general practitioners and hospital doctors; paramedics are already using them to provide faster diagnostics and better patient care. In trauma cases, a handheld ultrasound device can detect or verify the presence of free fluid in the peritoneum or thorax, facilitating immediate investigation and improving patient prognosis.
Numerous articles in PubMed and other databases advocate the use of POCUS. For instance, one study encourages non-cardiologists to utilize heart ultrasound. Combining ultrasound with clinical expertise can expedite clarification, validate or challenge diagnoses, and facilitate swift interventions. Another study showed that targeted examinations conducted by skilled ultrasound doctors had diagnostic utility in nearly half of all patients examined, with almost one in five experiencing a change in diagnosis.
Other studies highlight that emergency doctors have high accuracy in performing POCUS for suspected deep venous thrombosis (DVT) in the lower extremity, comparable to radiologists. They also performed assessments in an average time of three minutes. Ultrasound assessments for all lower extremity DVTs exhibited a sensitivity and specificity of 89%, while proximal lower extremity DVTs showed a sensitivity of 95% and specificity of 96%. Studies involving lung ultrasound and the kidney and urinary tract system show how medical professionals can confirm or negate conditions, reducing waiting times and delays in treatment.
For Focused Assessment with Sonography for Trauma (FAST) examinations, the primary goal in trauma patients is to identify intraperitoneal free fluid, allowing immediate transfer to higher levels of care. Various articles describe the advantages and disadvantages of this examination, with some studies showing no significant difference in diagnostic accuracy between radiologists and non-radiologists.
These studies underscore that ultrasound is a valuable tool for promptly diagnosing and implementing interventions, whether in a hospital or clinic setting. Quick access to ultrasound imaging can accelerate diagnosis and treatment, potentially saving lives.
POCUS is the use of ultrasound at the patient’s bedside for diagnostic and therapeutic purposes. The adoption of handheld ultrasound devices for POCUS offers numerous advantages. With handheld ultrasound, doctors can quickly gather critical information at the point of care, enhancing their diagnostic capabilities and improving patient outcomes. The immediacy and convenience of handheld ultrasound reduce the need for patient transport to imaging departments, increasing comfort and reducing wait times. By providing immediate visual information, POCUS enhances the clinician's ability to make timely and accurate decisions. For example, in trauma cases, POCUS can quickly identify internal bleeding or organ damage, guiding immediate intervention. The portable nature of POCUS devices, especially handheld ultrasound units, makes it possible to bring imaging capabilities to a wide range of settings, including remote locations, field hospitals, and during patient transport. Additionally, POCUS reduces the need for more expensive and time-consuming imaging modalities, such as CT scans or MRIs, particularly in settings where rapid decision-making is critical. This cost-effectiveness is particularly beneficial in resource-limited environments.
Learning to use handheld ultrasound and perform POCUS can significantly enhance a doctor's skill set. It allows for better integration of imaging into everyday clinical practice, improving overall diagnostic accuracy and patient management. Handheld ultrasound can streamline workflows by reducing the need for referrals and follow-up imaging, thereby increasing efficiency and reducing healthcare costs.
POCUS has numerous clinical applications. In cardiology, it is used to assess cardiac function, detect pericardial effusion, and guide resuscitation in cardiac arrest situations. In pulmonology, it helps evaluate pleural effusions, pneumothorax, and pulmonary edema. In gastroenterology, POCUS is used to identify free fluid in the abdomen, assess the gallbladder for cholecystitis, and guide procedures such as paracentesis. In obstetrics and gynecology, it is valuable for monitoring fetal development, assessing early pregnancy viability, and evaluating gynecological emergencies. In emergency medicine, POCUS is essential for the rapid assessment of trauma patients, diagnosing abdominal aortic aneurysms, and guiding vascular access.
The use of POCUS is expected to continue growing as more clinicians recognize its value in enhancing patient care. Technological advancements, such as the development of more affordable, high-quality handheld ultrasound devices, and the integration of artificial intelligence for image interpretation, are likely to further expand its applications and accessibility.
Ultrasound technology has evolved significantly from large, stationary machines to today's portable handheld devices. POCUS further enhances this technology, allowing clinicians to perform ultrasound exams at the patient's bedside, providing immediate diagnostic information crucial for emergency and critical care settings. POCUS improves diagnostic accuracy, patient outcomes, and clinical workflows, making it an indispensable tool in modern medicine due to its portability, cost-effectiveness, and broad range of applications.
References
1. Labovitz AJ, Noble VE, Bierig M, Goldstein SA, Jones R, Kort S, et al. Focused cardiac ultrasound in the emergent setting: a consensus statement of the American Society of Echocardiography and American College of Emergency Physicians. J Am Soc Echocardiogr. 2010;23(12):1225-30.
2. Mjolstad OC, Dalen H, Graven T, Kleinau JO, Salvesen O, Haugen BO. Routinely adding ultrasound examinations by pocket-sized ultrasound devices improves inpatient diagnostics in a medical department. Eur J Intern Med. 2012;23(2):185-91.
3. Blaivas M, Lambert MJ, Harwood RA, Wood JP, Konicki J. Lower-extremity Doppler for deep venous thrombosis--can emergency physicians be accurate and fast? Acad Emerg Med. 2000;7(2):120-6.
4. Fox JC, Bertoglio KC. Emergency Physician Performed Ultrasound for DVT Evaluation. Thrombosis. 2011;2011:938709.
5. Lichtenstein DA, Meziere GA. Relevance of lung ultrasound in the diagnosis of acute respiratory failure: the BLUE protocol. Chest. 2008;134(1):117-25.
6. Wimalasena Y, Kocierz L, Strong D, Watterson J, Burns B. Lung ultrasound: a useful tool in the assessment of the dyspnoeic patient in the emergency department. Fact or fiction? Emerg Med J. 2018;35(4):258-66.
7. Hew M, Tay TR. The efficacy of bedside chest ultrasound: from accuracy to outcomes. Eur Respir Rev. 2016;25(141):230-46.
8. Parulekar P, Neil-Gallacher E, Harrison A. Intensive care unit physician-delivered point of care renal tract ultrasound in acute kidney injury is feasible. J Intensive Care Soc. 2018;19(4):313-8.
9. Nepal S, Dachsel M, Smallwood N. Point-of-care ultrasound rapidly and reliably diagnoses renal tract obstruction in patients admitted with acute kidney injury. Clin Med (Lond). 2020;20(6):541-4.
10. Dolich MO, McKenney MG, Varela JE et-al. 2,576 ultrasounds for blunt abdominal trauma. J Trauma. 2001;50 (1): 108-12.
11. Natarajan B, Gupta PK, Cemaj S et-al. FAST scan: is it worth doing in hemodynamically stable blunt trauma patients?. Surgery. 2010;148 (4): 695-700.
12. Bhoi S, Sinha TP, Ramchandani R et-al. To determine the accuracy of focused assessment with sonography for trauma done by nonradiologists and its comparative analysis with radiologists in emergency department of a level 1 trauma center of India. J Emerg Trauma Shock. 2013;6 (1): 42-6.
13. Keila G Carrera, Gashaw Hassen et. The Benefits and Barriers of Using Point-of-Care Ultrasound in Primary Healthcare in the United states. Cureus. 2022 Aug; 14(8): e28373.
14. Hashim Ahmed, Tahir Muhammad Junaid. The utility of point of care ultrasonography (POCUS). Ann Med Surg (Lond). 2021 Nov; 71: 102982.
15. Courteney D.M. Fraleigh, BN et. Point-of-care ultrasound: An emerging clinical tool to enhance physical assessment. Nurse Pract. 2022 Aug; 47(8): 14–20.