AI and IoT integration in the healthcare industry offers exciting possibilities for transforming patient care and the healthcare industry as a whole. As these technologies continue to evolve, it is crucial to address challenges and ethical considerations to ensure a positive and equitable impact.
Before we go into the details of the Internet of Things and Artificial Intelligence. We should cover some basic points that illustrate the enormous challenges and opportunities facing global healthcare systems.
On the challenges side, United Nations projections indicate that the over 65 years of age is projected to rise to over 1.6 billion by 2050. Placing unprecedented strain on already overstretched healthcare systems.
On the opportunities side we are seeing tremendous innovation on the level of individual sensors in terms of precision, continuity and comfort. Also the total amount of IoT sensors is estimated to grow nearly 1.5 billion by 2030.
The current generation of sensors available in non-hospital consumer devices such as smart watches or smart bracelets lacks safety and accuracy with a host of reliability and security issues. An example by Smith et al. 2023 take sleep measurement by consumer devices as an example of this.. Smart watches are too unreliable and inconsistent to create valid Artificial Intelligence-based learning models while using smart bracelets results in the loss of large amounts of data.
The solutions to this come from both the inherent sensor technology and the AI-based algorithms. A review by Vaghasiya et al. 2023, outlines the new-generation of hospital-grade sensors. The following graphic is from that review. (Figure 1)
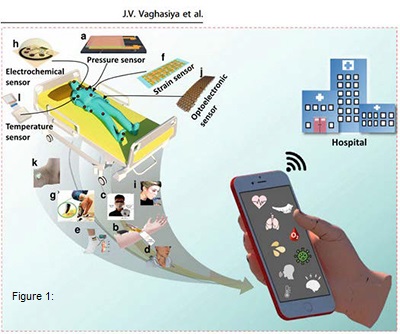
On the AI-algorithm side Smith et al. 2023, notes that algorithms need to be tailored to the general characteristics of specific disease categories in order to reduce false positives. Then using support vector machines such as LASVM, ISVM, and K-prototypes clustering, algorithms can be generated which reduce false signals but that is also accurate.
Smith et al. 2023 notes the example of a wearable sensor for knee osteoarthritis patients that calculates optimal exercise intensity.
A review by Chen et al. 2023, provides a short overview of issues regarding the security and privacy of IoT wearable sensors. The issues of security and privacy are very real and pose an even greater threat to vulnerable patient populations such as the elderly.
According to a review by Dayan et al 2021, “Federated Learning is a method used to train AI models on disparate data sources, without the data being transported or exposed outside their original location.”
Also, in the Dayan et al. 2021 review a client-server technique is discussed.
“The client-server sends an ‘untrained’ model to other servers (‘nodes’) that conduct partial training tasks, in turn sending the results back to be merged in the central (‘federated’) server. This is conducted as an iterative process until training is complete.”
In these cases, only the model weights and gradients are communicated between client sites and federated servers.
Looking at the sector we can note two types of regulation. On one side efforts from industry participants and academia themselves and on the other side regulation by government bodies.
With regard to efforts from the industry, we can note the EQUATOR Network’s efforts in the realm of creating reporting guidelines for prediction models and algorithms.
This checklist is called TRIPOD and can be found openly via the following link: https://www.tripod-statement.org/resources/
With this industry tries to create a more homogenous playing field with regard to algorithms including AI and deep learning.
Regulation of AI, algorithms, and hospital-grade medical devices are regulated by the European Union by the European Medical Agency. In the European Union all medical devices if they are to be used legally must have a so-called CE (Conformité Européenne) mark on the device or algorithm to note that it has passed certain conformity tasks.
In the United States, the FDA also regulates AI algorithms and hospital-grade IoT wearable’s under their medical device regulations.
That regulation is necessary is something everyone agrees on to maintain standards and levels because of the unique nature of medical algorithms and devices.
The following infographic from “Medical Futurist” shows that despite regulation there are now hundreds of algorithms available for medical professionals in nearly all specialties. (Figure 2)
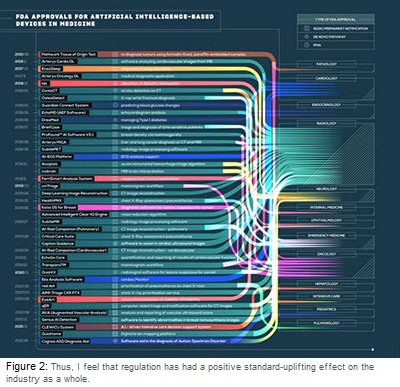
The greatest opportunities for AI and IoT lies in the continuous and longitudinal assessment of real-time patient data. Combined with instantaneous alarms when an emergency such as a heart attack or stroke does arise.
The opportunities are vast, from predicting disease events before they occur through predictive algorithms, potentially preventing an entire disease event such as a heart attack and saving enormous amounts of human suffering and monetary resources. Also, remote care for underprivileged rural area inhabitants.
In the review by Chen et al. 2023 the concept of a complete “Smart Home” for geriatric patients was discussed. The following graphic is from that review. (Figure 3)
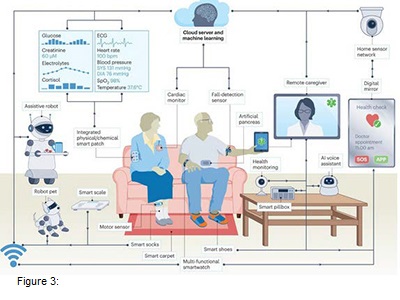
This is an enormously complex topic where the industry and regulators are still seeking to catch up with the large progress enabled by technology.
The World Health Organization has recently published a guideline for the healthcare sector entitled “Ethics & Governance of Artificial Intelligence for Health” (https://www.who.int/publications/i/item/9789240029200)
Key points discussed in this extensive guidance report are:
- Human Rights to Health
- Data protection laws and policies
- Principles for use of AI in healthcare
- Bioethics laws and policies
- Regulatory considerations
With regard to ethics, key considerations are standards for human supervision, human warranty, and the evaluation of models by humans and clinicians. Also, the informed consent process has to be rigorously followed.
Looking at regulations many organizations are currently in the process of drafting updated guidance for these technologies in the coming years. As an industry key points will be data privacy adherence, security, and especially good clinical validation of AI models before they enter healthcare sphere.
In general we have to state that the healthcare sector as a whole is the sector which will see the most demand for jobs in the United States according to a recent McKinsey report.(Figure 4)
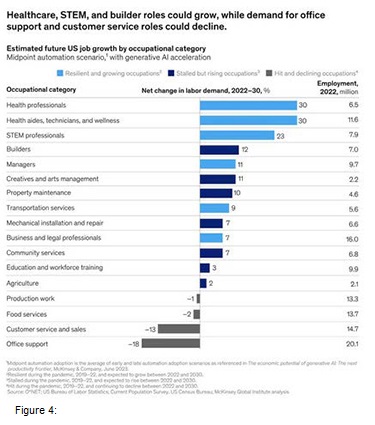
This report estimates that the sector will see a shortage of 3.5 million jobs in the near future mainly due to aging population demographics.
That being said the topic of AI and automated IoT sensor technology does raise the very valid point with regards to the job security of individual jobs. Especially if in the future it becomes the case that an AI-algorithm might be better suited at specific scenarios than human practitioners. In this case it might even become unethical to have humans doing certain tasks.
What is especially crucial to understand that physicians take more than a decade of intense education to be trained for their roles? As a result this group might be much more difficult to re-task and retrain these professionals to take over novel roles that will be simultaneously created by the AI&IoT revolution.
Those most at risk for displacement long-term are both on the extreme specialization end. Such as specialist radiologists, pathologists, and ophthalmologists. Mostly the image-based diagnosis specialties. On the other end, much simpler healthcare professions such as those doing routine patient controls, data-entry professions and costumer services will also most certainly be automated.
What best to do in this complex case of job displacement, is to have active life-long learning trajectories and to use these professionals as educators for future medical physicians in a university role.
With regards to IoT sensors, novel two-dimensional materials with improved flexibility, enhanced mechanical stability, high sensitivity, and excellent accuracy are already being developed and are now ready to enter the clinics.
Looking at security & privacy, blockchain cryptography, and a later stage Quantum Computing based encryption offer tantalizing potential albeit Quantum computing is still some ways off from being deployable for these purposes. But blockchain and smart contract technology is already being deployed by various parties within the healthcare sector.
Lastly, artificial intelligence the development of enhanced computing technology either through specialized semiconductor chips, novel techniques to decrease LLM-based computing needs, and the ever-increasing total global cloud computing infrastructure makes the future of AI in general and especially in the ultra-complex healthcare sector very bright indeed.
References
1. Smith, A.A., Li, R. & Tse, Z.T.H. Reshaping healthcare with wearable biosensors. Sci Rep 13, 4998 (2023). https://doi.org/10.1038/s41598-022-26951-z
2. Vaghasiya, J.V., Mayorga-Martinez, C.C. & Pumera, M. Wearable sensors for telehealth based on emerging materials and nanoarchitectonics. npj Flex Electron 7, 26 (2023). https://doi.org/10.1038/s41528-023-00261-4
3. Chen, C., Ding, S. & Wang, J. Digital health for aging populations. Nat Med 29, 1623–1630 (2023). https://doi.org/10.1038/s41591-023-02391-8
4. Dayan, I., Roth, H.R., Zhong, A. et al. Federated learning for predicting clinical outcomes in patients with COVID-19. Nat Med 27, 1735–1743 (2021). https://doi.org/10.1038/s41591-021-01506-3